Case Study
Superior Vision
Provider Portal
Redesigning the secure provider portal for a national vision care plan — from a fragmented legacy system to a self-serve platform that supported a billion-dollar acquisition.
1B+
METLIFE ACQUISITION VALUE
4
DISTINCT USER TYPES
Millions
MEMBERS & PROVIDERS
HIPAA
PII COMPLIANT
CLIENT
Superior Vision
SECTOR
Healthcare / Managed Vision Care
The Challenge
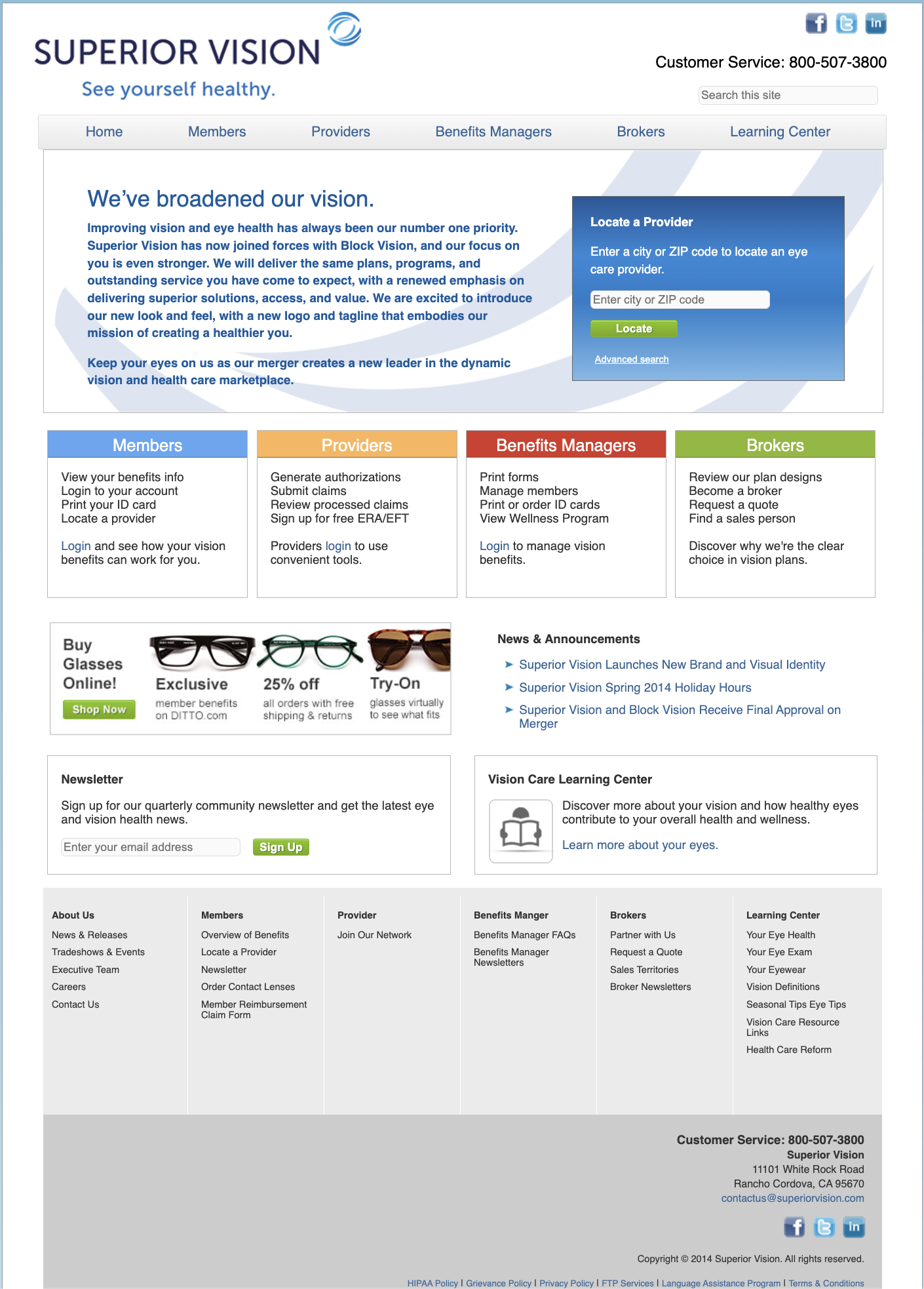
A Platform Built for Four Audiences — With One Broken Experience
Superior Vision had been a leader in managed vision care since 1993, providing routine PPO vision plans to employers across the nation. Their provider portal served four distinct user types — members, providers, employers, and internal staff — but the legacy system had never been built to serve them distinctly. A Flash-dependent homepage offered icon-based navigation with no clear task direction, and providers were abandoning the portal for the phone.
“With a MetLife acquisition on the horizon, the stakes were high. The platform needed to demonstrate scalability, compliance, and user confidence to a billion-dollar buyer — not just look better.”
I led the requirements gathering and redesign effort with HIPAA compliance and PII protection as non-negotiable constraints throughout every phase.
My Approach
Mapping Four User Types to One Coherent Platform
- Multi-audience requirements elicitation — Gathered and documented requirements for each of the four user groups, covering eligibility verification, authorization workflows, claims submission, and self-service support — surfacing conflicts and overlaps across user roles.
- Permission matrix & compliance documentation — Defined what each user type could view, create, and modify. Documented HIPAA-aligned permission rules as functional requirements to ensure PII was protected throughout.
- Pain point analysis — Worked with providers and members to map the specific friction points driving portal abandonment. Key finding: users couldn’t identify their workflow path from the homepage, and high-frequency tasks were buried behind excessive navigation steps.
- UX redesign — Translated requirements into a redesigned homepage that surfaced each of the four user type pathways immediately, replacing the Flash intro with clear, task-oriented navigation anchored in user research.
- Developer collaboration & compliance validation — Partnered with the development team to ensure correct implementation of HIPAA-compliant data handling across all form submissions and views.
Key Deliverables
What I Produced
- Multi-audience requirements elicitation — Gathered and documented requirements for each of the four user groups, covering eligibility verification, authorization workflows, claims submission, and self-service support — surfacing conflicts and overlaps across user roles.
- Permission matrix & compliance documentation — Defined what each user type could view, create, and modify. Documented HIPAA-aligned permission rules as functional requirements to ensure PII was protected throughout.
- Pain point analysis — Worked with providers and members to map the specific friction points driving portal abandonment. Key finding: users couldn’t identify their workflow path from the homepage, and high-frequency tasks were buried behind excessive navigation steps.
- UX redesign — Translated requirements into a redesigned homepage that surfaced each of the four user type pathways immediately, replacing the Flash intro with clear, task-oriented navigation anchored in user research.
- Developer collaboration & compliance validation — Partnered with the development team to ensure correct implementation of HIPAA-compliant data handling across all form submissions and views.